Most of us have heard of varicose veins and know what they look like, but how can they be treated? More importantly, should you see a vascular doctor for varicose veins?
“Varicose veins do not pose a health threat,” says Adam B. Levitt, M.D., a board certified vascular surgeon at Vascular Specialists of Central Florida. “Why should someone see a vascular doctor for varicose veins?
People may not like the way their legs look and want something done. That’s a very valid reason to have your veins treated.”
What Are Varicose Veins?
Varicose veins show up commonly in the legs as enlarged, twisted, bulgy, bluish-purple contortions just under the surface of the skin. They can be minimal in appearance or appear as large, rope-like structures.
Normally, one-way valves in the leg push blood up toward the heart to keep blood circulation flowing freely. If these valves fail, blood will back up, causing the veins to swell — which can result in discomfort, aches, and cramping.
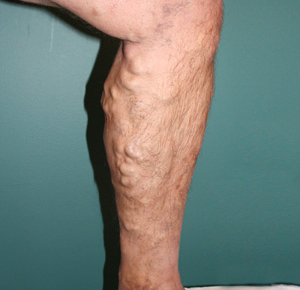
Example of varicose veins before treatment.
Patients may have difficulty standing up for an extended time and develop swollen ankles and skin blemishes if their varicose veins become bad enough. In severe circumstances, a varicose vein may rupture or an ulcer may surface on the skin. “Varicose veins can cause patients problems simply cosmetically,” says Dr. Levitt. “Some patients will complain of tired, achy legs, or of a discomfort in their legs. Some varicose veins will bleed, some will have leg swelling or color changes in their legs.”
Indeed symptoms caused by venous insufficiency can include nagging, throbbing leg pain,
leg fatigue, and leg heaviness, all of which may get worse during the day. Many individuals will need to sit down and elevate their legs later in the day to alleviate the symptoms.
In extreme circumstances, varicose veins can cause serious skin discoloration and even ulceration. “Worse case scenario, people will have ulcers in their legs,” confirms Dr. Levitt. “If any of these symptoms sound familiar, please come and see us so we can evaluate your different treatment options.”
Varicose Veins Risk Factors
Medical sources estimate that roughly 20% of adults in the United States have varicose veins. Other factors increasing the risks of developing varicose veins include:
- Family history
- Gender (women are more prone to developing varicose veins than men)
- Being pregnant
- Old age
- Traumatic leg injuries
- Obesity
- Reduced mobility
Treatment Options for Varicose Veins
 Some individuals aren’t concerned by the sight of varicose veins and don’t feel any discomfort or other symptoms. In that case, their vascular surgeon may recommend certain lifestyle changes, like increased exercise, weight loss regimes, and refraining from wearing tight-fitting clothes.
Some individuals aren’t concerned by the sight of varicose veins and don’t feel any discomfort or other symptoms. In that case, their vascular surgeon may recommend certain lifestyle changes, like increased exercise, weight loss regimes, and refraining from wearing tight-fitting clothes.
However, if symptoms do present themselves, treatment options exist to relieve pain, skin coloration, blood clots or other problems.
Common treatments for varicose veins include:
- Compression stockings
- Raising the leg for extended periods of time
- Regular exercise
- Diet modification
When nonsurgical treatments fail, other longer-lasting treatment options may include:
- Laser treatment
- Injections
- Ablation therapy (closing the veins or taking them out altogether)
The majority of surgical treatments are done on an outpatient basis, in the vascular surgeon’s office, and are usually completed in about an hour.
